What is Anthrax?
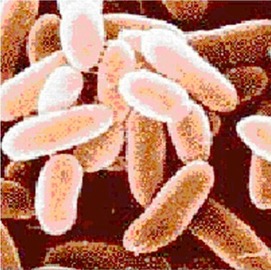
Anthrax is a serious, life-threatening, infectious disease caused by the gram-positive, spore-forming bacteria called Bacillus anthracis. Under the microscope, these bacteria appear like large rods. Once they’re in the soil, where they live, this organism becomes dormant and forms into a spore. These spores are very difficult to destroy and are known to survive in the soil for more than 40 years.
Anthrax normally affects animals, especially goats, cattle, sheep and horses. Infection in humans was initially non-existent in industrialized nations, but not until the threat of bioterrorism became evident in the late 2001. This disease can be transmitted to humans through contact with infected animals, products from infected animals, and intentionally tainted materials. Anthrax, however, does not spread from person to person.
Like any other infectious disease, the incubation period (time between contact with anthrax and the start of symptoms) for anthrax varies, and it may take more than a week before an infected person begins to manifest the symptoms.
How Can Anthrax Infect Humans?
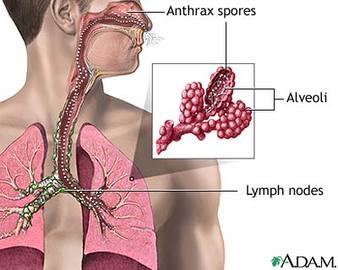
Anthrax is a potent biological weapon because spores can be spread easily through the mail or other means. This disease can infect humans in three ways. People who are exposed to airborne particles may develop cutaneous, inhalation, or gastrointestinal anthrax, depending on the route of exposure.
The most common form of infection is cutaneous anthrax. After an incubation period of 1 to 12 days, an ugly sore appears, one that may develop into a necrotic ulcer. In some cases, however, the sore will just disappear on its own even without treatment. Other symptoms of cutaneous anthrax include fever, malaise and headache. There may also be involvement of the lymph nodes.
Gastrointestinal anthrax occurs approximately 1 to 7 days after ingestion of contaminated food or undercooked contaminated meat. This can cause a serious, sometimes fatal disease. Symptoms include nausea, loss of appetite, fever, severe abdominal pain, bloody vomiting, and bloody diarrhea. The oropharyngeal form may also occur, manifested by lesions at the base of the tongue, difficulty swallowing, fever, and enlargement of the cervical lymph nodes.
The most fatal form is inhalation anthrax. After an incubation period of several days to 60 days, the infected person may manifest symptoms such as a brief prodromal fever, cough, fatigue, and mild chest discomfort that may quickly progress to severe respiratory distress, sweating, stridor, cyanosis and signs of meningitis (rigidity of the neck, headache, photophobia, altered mental state). If left untreated, it may proceed to shock and after 24 to 36 hours, death may ensue.
How to Diagnose Anthrax
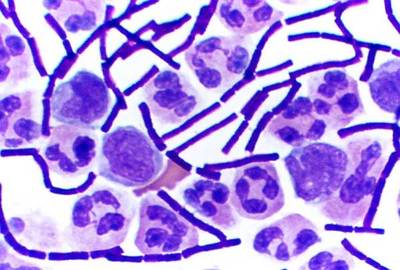
Tests to diagnose anthrax depend entirely upon the type of disease that is suspected. History-taking, including the person’s occupation, is essential in determining infection. Nasal swab testing may be conducted on several individuals to detect the presence of anthrax in the environment, although this does not confirm infection by anthrax in a person. The bacteria may be found in cultures or smears in cutaneous anthrax or sputum cultures in inhalation anthrax. Chest X-ray or Chest CT scan may also show significant changes in and between the lungs. Once the anthrax spreads inside the body, bacteria can be seen in blood using a microscope. Additional diagnostic tests include spinal fluid cultures (before antibiotics) and polymerase chain reaction testing.
Management and Treatment
Antibiotic prophylaxis after exposure to anthrax spores is necessary, and a 60-day therapy is strongly advised. Several antibiotics are effective, including ciprofloxacin, doxycycline, penicillin and amoxicillin (if penicillin sensitivity of organism is confirmed).
Treatment of cutaneous anthrax includes a 60-day therapy using the abovementioned antibiotics; however, signs of systemic involvement, including lesions of the head and neck and widespread edema require intravenous therapy with multiple drugs, especially in the case of inhalation anthrax.
Treatment of inhalation, gastrointestinal and oropharyngeal anthrax requires intensive care and supervision, along with the administration of two or three intravenous antibiotics. Intravenous therapy can then be switched to oral antibiotic therapy if clinical improvement is noted. Total therapy is 60 days.
There are two principal ways to prevent anthrax. For people who have been exposed to anthrax but remain asymptomatic, doctors may prescribe preventive antibiotics like ciprofloxacin, penicillin or doxycycline, depending on the anthrax strain.
Also, an anthrax vaccine has been available to veterinarians, animal product handlers at high risk for exposure, U.S. military personnel and other members of the general public. It is a six-dose series that requires yearly boosters. However, its role in routine prophylaxis and adjunct treatment remains to be an issue. Refined vaccines are still being developed.
A Few Helpful Interventions
- In severe cases (for all forms), intravenous corticosteroids may be administered as adjunct therapy.
- Treatment of symptoms includes administration of analgesics, antiemetics and emergency drugs for circulatory collapse.
- Monitor vital signs and hemodynamic parameters thoroughly for circulatory collapse and during antibiotic therapy.
- Provide supplemental oxygen or mechanical ventilation as needed.
- Anthrax is a reportable disease. Advise the infected individual and his family that a public health official will investigate the case for source of infection.
Comments
Most Recent Articles
-
How To Prevent Imha
Your pets too can acquire disease like you. Some of these diseases may be those common ones or those that are serious in nature. Like people, dogs also have their own immune system. Our immu...
-
the Most Common Zoonotic Disease
You may not be familiar or would have never heard the term Zoonotic diseases, but yes they exist. These are infectious diseases transmitted from animals whether wild or domesticated, to huma...
-
Leadng Causes Of Cancer in Men
Cancer knows no gender. Even the bravest of men can be affected by men cancer. Cancer can come to any man in many different forms. Certain types of cancer may show some signs of its possible...
-
What Are The Causes Of Blackleg
Sheep are the most common target of blackleg disease, also known as Clostridium chauvoei. The blackleg disease was derived from the infected part of the sheep which is usually the leg, ...
-
what is psittacosis?
What is psittacosis? It is one of the zoonotic infectious diseases caused by a bacterium called Chlamydophila Psittaci. Psittacosis is also called parrot fever or chlamydiosis. The name of t...
-
Bloating And Digestive Diseases
There are many people who experience digestive diseases due to different causes. There are many reasons why one’s digestive system acquires these diseases. But the important thing to c...
-
What You Must Know About Medical Diseases
Most people have experienced some kind of a disease before or at least at one point in life. And if you can still remember the last time you suffered from a disease and felt ill, you will re...
-
What Deseases Are Caused By Low Vitamin Intake
People who have low vitamin intake may cause often deseases and low immune system. Vitamins and minerals are usually comes from the food we eat such as green leafy vegetables, fruits an...
-
How To Treat Neglected Tropical Diseases
Neglected tropical Diseases (NTD) are a group of bacterial and parasitic infections which are affecting 1 billion people. Studies show that these infections persist exclusively in the poores...
-
How To Prevent Psoriasis Skin Diseases
You might have heard of this disease before but have less or no idea of what this is all about. If you are one of those who are experiencing this type of skin disease or just want to know mo...
-
What Makes the Body Succumb To Cancer
Cancer comes in different types, different stages and different succumb to our body. When the type of cancer is in an early stage, the person may not be aware of his disease. Medical treatme...
-
What Stops Disease Outbreaks From Spreading To Everyone?
Although it is not common that we hear experts and those in authority call an outbreak on something, hearing this word is not something we would want. Outbreaks are often associated with dis...
-
What Are the Symptoms Of Liver Cancer?
Hepatocellular carcinoma or liver cancer as it is commonly known arises from the liver. The human liver is composed of a number of different cell types such as bile ducts and blood vessels b...
-
What Is Bladder Cancer?
The urinary bladder plays a vital role in the human body and its functions. The bladder is a muscular sac in the pelvis where fluid or urine from the kidneys is stored. During urination the ...
-
What Is Bone Cancer?
Our body is composed of 206 bones from head to toes and when abused may cause bone cancer. Bone cancer is a disease that eats-up the components of the bone inside the body. In may start from...